Eating disorders require recognition as serious mental illnesses with significant physical health consequences and risks, that generally require the involvement of both the mental health and medical service systems. Describing how these systems of healthcare work together as a tiered pyramid is a common approach:
“related to the complexity and severity of the mental health problems, and to the appropriate service response, relevant care pathways and service links”. Australian Government (2004)
Tier One Services– Primary care
Who: Person who is at risk of developing an eating disorder who comes to the attention of someone they have a direct relationship with, and who is in a position to intervene, but does not necessarily have specialist mental health training.
Role: Support the person to help them manage and reduce the signs of a developing eating disorder such as disordered eating, an increase in activity/exercise or food-related behavioural or social change. This is also an early opportunity to provide information and support to the families of the person with the eating disorder.
Such supports have a major role in dealing with the mental health of most people and in facilitating the person accessing tier 2, 3 and 4 services if required.
In partnership with specialist practitioners in tiers 2 and 3, they may help address uncomplicated mental health problems, through prevention and mental health promotion, early intervention, case identification, and referral.
Supports/Services:
- informal supports, including parents, family, partners, teachers, employers, colleagues, and friends;
- health sector services, including general practitioners, community health centres, and services;
- health and wellbeing staff within the education sector, including schools and TAFE colleges;
- community services and agencies, including a range of community-based youth and welfare services, Centrelink, homelessness agencies, youth workers, cultural organisations, workplaces, sports clubs; and
- juvenile justice health services and child protection and care services.
Tier Two Services – Generalist health services
Who: People who have identified disordered eating that is developing into a diagnosable eating disorder such as Bulimia Nervosa, Binge Eating Disorder or OSFED conditions will require a referral to professionals and services that have some mental health training and expertise.
Role: Interventions at this level are provided in the community and tend to focus on assessing the problem and finding and referring to appropriate treatment and support options for the person with an eating disorder. It is important at this service delivery level to provide the family with ongoing support and information, including a formal care and support plan.
Support/services: General practitioners with extra mental health training, physicians, paediatricians, dietitians, headspace, private psychologists, counsellors, nurses, psychologists, social workers, medical registrars, private psychiatrists, occupational therapists, MHCSS services, drug and alcohol workers, and other health professionals.
Tier Three Services – Specialist community based services
Who: A person who has been diagnosed with Anorexia Nervosa, ARFID etc. will require care at the tier three level.
Role: Involves multidisciplinary team approaches and are provided by community based or outpatient specialist eating disorders services in the public or private sector.
The types of intervention and care may be similar to those of tier two services, but the focus is on more complex cases or specific and enduring problems that need the skills of a multidisciplinary and more specialised mental health team
Supports/services: Services and health professionals involved include CAMHS/CYMHS, Adult MHS, eating disorders specialist services outpatient programs, public and private psychiatrists, physicians, paediatricians, specialist mental health nurses, dietitians, clinical psychologists, social workers, occupational therapists and others with specialised eating disorders training.
Tier Four Services – Specialist inpatient and emergency services
Who: If the eating disorder and its physical or mental health complications are severe enough, inpatient units may be required for intensive acute care.
Role: To contain, stabilise and manage severe problems, until the difficulties can be successfully managed at a less intensive tier 3 level.
Supports/services: Admission to a general mental health or medical unit within the hospital, or to a specialist eating disorders inpatient unit. For many people entry to the tier 4 inpatient services is via the emergency department. For some, this is their first presentation for help.
Coordinated System of Care
The person’s level of acuity and risk requires an assessment to determine the appropriate levels and intensity of care from services across all tiers of the healthcare system, supported by communication between, and transitions through the tiers of the system based on need and risk.
The outcomes of a well-resourced, coordinated and seamless four-tier service structure would ensure:
- early identification of an emerging eating disorder in tier one and/or tier two services, resulting in immediate access to early intervention treatment and support services to ensure optimal recovery and prevent the escalation of the condition and the resultant need to access tier three and four services;
- clarity about the criteria and pathways for admission into mental health and/or medical inpatient units as well as eating disorders specialist services;
- clear indicators of when tier one and tier two services need to escalate the person’s care and refer them to tier 3 and/or tier 4 services; and
- services in tier 1 and 2 would have seamless access to clinical and service decision-making consultation with services in tier 3 and tier 4.
The following figure summarises the service types within the four tiers identified by stakeholders who participated in the service mapping activities.
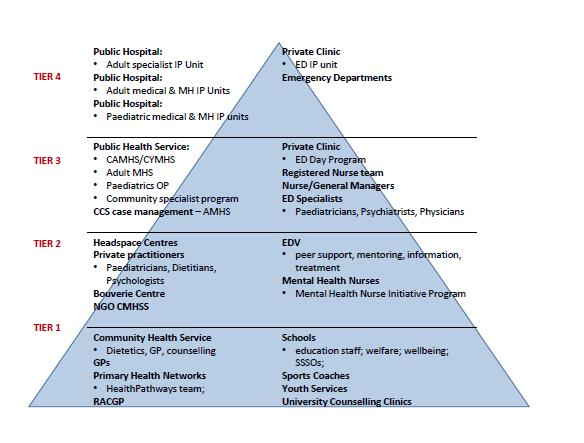
Reference:
Australian Government, 2004, Responding to the mental health needs of young people in Australia: discussion paper: principles and strategies, Department of Health.
